Best candidates: ≤10–15 mm renal/upper ureter stones with HU ≤1000 and favorable anatomy.
Lower pole: evaluate IPA, infundibular length/width; SWL works if drainage is favorable.
Challenging: very hard stones (HU >1000–1200), large burden, unfavorable lower-pole anatomy, severe obesity (targeting/coupling), skeletal deformity.
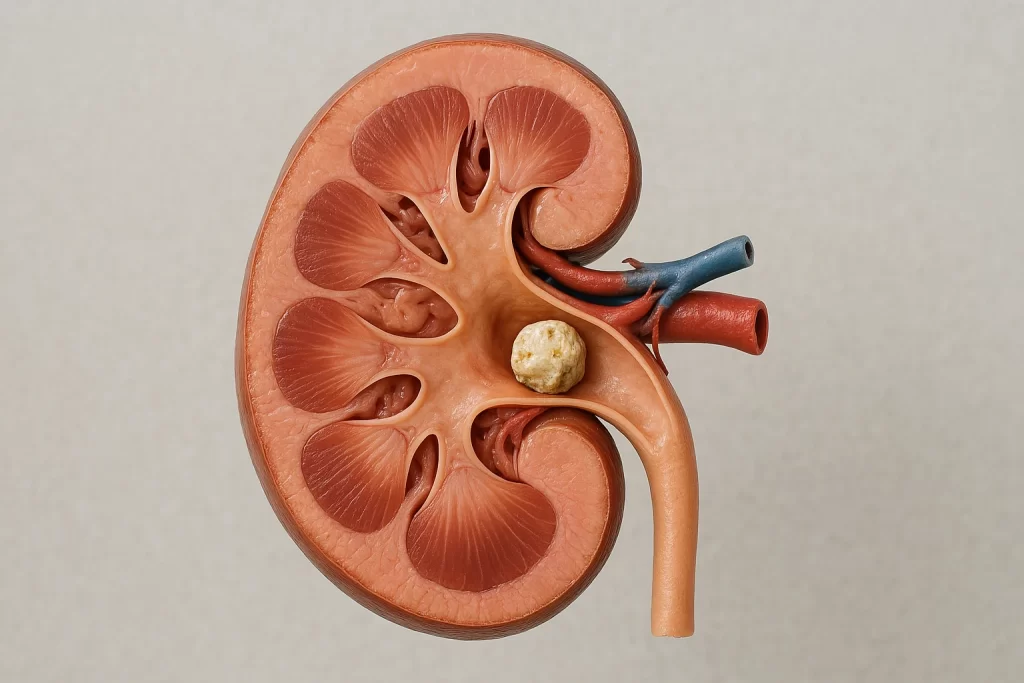
Imaging: NCCT (size, side, HU, skin-to-stone distance), note anatomy.
Labs: UA/UCx if symptomatic; treat infection before SWL.
Medicines: pause/bridge anti-coagulants per policy; α-blocker plan for distal ureter stones or heavy fragment load.
Analgesia: multimodal; ensure patient can breathe normally for stable targeting.
Consent & Counseling: colic, hematuria, steinstrasse risk; hydration plan.

Use liberal gel, remove micro-bubbles, avoid dry “hot spots.”
Re-apply after any reposition.
If using a membrane/balloon interface, check for folds or trapped air.
Prefer inline/iso-centric alignment of imaging axis and shock path when available.
Re-center with every respiratory cycle initially; coach shallow breathing.
Use ultrasound or fluoro as primary; swap if visibility drops (e.g., bowel gas, bone overlap).
Pause to re-target after any patient movement.

Principles

Fragment plume/contrast change → positive sign; continue at current settings.
No progress after 300–500 shocks: re-image; check coupling; try lower frequency or slight energy increase; ensure true focus on stone.
Arrhythmia/pain: switch to ECG-gating if available; reduce energy/frequency; reassess.

Pediatrics: favor fine energy graduation (small step sizes), meticulous coupling, and low-frequency priming; minimize fluoroscopy, prefer US when feasible.
Obese patients: anticipate higher skin-to-stone distance—optimize gel pool, consider US targeting; adjust table focus depth; manage respiratory motion.
Anticoagulation risk / solitary kidney: stricter injury threshold; maintain conservative ramp; close post-op monitoring.

Renal hematoma: slow ramp, avoid unnecessary max energy, control BP, ECG gating if ectopy.
Steinstrasse: counsel high hydration; consider α-blocker for high fragment load; schedule timely follow-up.
Infection/sepsis: ensure pre-SWL urine sterility; abort if fever/chills.

Hydration + analgesia.
Strain urine and log passage.
When to call: fever, refractory pain, anuria.
Follow-up imaging: timeframe based on size/site (commonly 2–6 weeks).
Next steps if residuals: repeat SWL vs. URS based on size, location, patient preference, and anatomy.

Poor visualization: switch modality; adjust patient tilt; treat bowel gas (positioning).
No fragmentation: re-center, improve coupling, drop frequency, modest energy uptick.
Pain limits ramp: pause, re-gel, analgesia top-up, resume at lower frequency.
Step-by-step guide for safe and effective energy escalation during SWL.
Quick pre-procedure reference to ensure readiness, safety, and accuracy.
Simple patient instructions for recovery, hydration, and follow-up after SWL.

Lithotripsy Academy is an educational initiative of Endourology Academy, focused on advancing knowledge and training in Shock Wave Lithotripsy (SWL) through evidence-based learning and clinical expertise.
Sign up for our newsletter to enjoy free marketing tips, inspirations, and more.